Ulcerative colitis (UC) is a chronic inflammatory bowel disease that affects the large intestine. It causes inflammation and sores in the lining of the colon, which can lead to severe pain, diarrhea, and other gastrointestinal symptoms. While there is no cure for UC, it is manageable with proper care and treatment.
we will discuss some useful tips for managing UC flare-ups
One of the most challenging aspects of living with UC is managing flare-ups. Flare-ups are periods when the disease is more active, and symptoms are more severe. In this article, we will discuss some useful tips for managing UC flare-ups, including lifestyle changes, medical treatment, and when to seek medical attention.
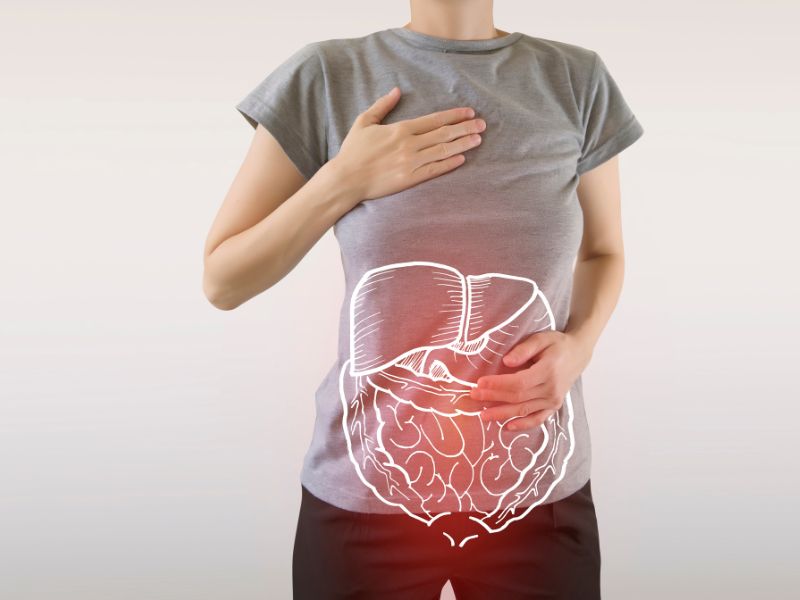
Understanding Ulcerative Colitis Flare-ups
Before we dive into the tips, let’s take a closer look at what flare-ups are and what triggers them. A flare-up is a sudden worsening of UC symptoms, such as abdominal pain, diarrhea, rectal bleeding, and fatigue. Flare-ups can last for days or weeks, and they can be unpredictable.
The triggers of UC flare-ups vary from person to person, but some common ones include stress, dietary changes, infections, and medications. It’s crucial to identify your triggers to avoid or manage them effectively.
Diet and Lifestyle Changes to Manage Ulcerative Colitis Flare-ups
Certain foods can trigger UC flare-ups, and it’s essential to avoid them during periods of disease activity. The foods to avoid with colitis may include spicy foods, high-fiber foods like nuts and seeds, fatty foods, and dairy products. It’s recommended to keep a food diary to identify specific foods that worsen your symptoms and eliminate them from your diet.
Anti-inflammatory foods can help reduce inflammation and prevent UC flare-ups. Some examples of anti-inflammatory foods include fatty fish like salmon, leafy greens like spinach, berries like blueberries, nuts like almonds, and seeds like chia seeds. These foods contain antioxidants and omega-3 fatty acids, which have anti-inflammatory properties.
Stress reduction techniques such as meditation, yoga, and deep breathing exercises can help manage stress and prevent flare-ups. Regular exercise can also improve UC symptoms by reducing inflammation and enhancing mood. Even low-intensity activities such as walking or cycling can be beneficial.
Probiotics, which are live bacteria that can restore the balance of good and bad bacteria in the gut, may also help manage UC flare-ups. It’s crucial to consult with your healthcare provider before trying any alternative therapy, as some may interact with medications or cause adverse effects.
Tips for Managing Ulcerative Colitis Flare-ups
Ulcerative colitis (UC) is a chronic autoimmune disease that can lead to inflammation, ulcers, and severe abdominal pain. UC flare-ups can be triggered by various factors such as stress, diet, and medication. There are various tips and strategies for managing UC flare-ups, including medication management, lifestyle adjustments, alternative therapies, and coping strategies.
Medications such as anti-inflammatory drugs, immunosuppressants, and biologics can reduce inflammation and relieve symptoms. As mentioned earlier, lifestyle adjustments such as dietary changes, stress reduction techniques, and regular exercise can also help manage UC flare-ups. Alternative therapies such as probiotics, acupuncture, and herbal remedies may also be helpful. Coping strategies such as self-care practices and social support can help alleviate discomfort and promote healing.
It’s essential to work closely with healthcare providers to determine the best treatment plan for each individual’s unique situation. Identifying triggers and developing personalized management strategies can help reduce inflammation, alleviate symptoms, and improve the overall quality of life for people with UC.
Related Posts
Medical Treatment Options for Ulcerative Colitis Flare-ups
The medical treatment options for UC flare-ups include medications and surgery. Anti-inflammatory drugs such as mesalamine, sulfasalazine, and corticosteroids can help reduce inflammation and alleviate symptoms. Immunosuppressants such as azathioprine, methotrexate, and cyclosporine can suppress the immune system and prevent inflammation.
Biologic drugs such as infliximab, adalimumab, and vedolizumab are used to target specific molecules involved in inflammation and improve symptoms. However, these medications may increase the risk of infections and other side effects.
If medications are ineffective or if the UC becomes severe, surgery may be necessary. The most common surgical option is colectomy, which involves removing the entire colon and rectum. In some cases, ileostomy or pouch surgery may be necessary.
It’s important to work closely with a healthcare provider to determine the best treatment plan for your unique situation, as there are potential side effects and risks associated with each medication and surgery. With proper management, many people with UC can achieve remission and maintain a good quality of life.
When to Seek Medical Attention
It’s essential to seek medical attention if you experience symptoms of ulcerative colitis (UC), such as abdominal pain, diarrhea, rectal bleeding, and weight loss. These symptoms can indicate a flare-up or progression of the disease.
In addition, seek medical attention if you experience severe symptoms such as high fever, severe abdominal pain, dehydration, or persistent vomiting. These symptoms may indicate a more serious complication of UC, such as toxic megacolon or bowel perforation.
It’s also important to have regular check-ups with your healthcare provider to monitor your UC and adjust your treatment plan as needed. Routine monitoring can help detect flare-ups early and prevent complications.
If you are experiencing mental health issues such as anxiety or depression related to your UC, it’s crucial to seek mental health support and counseling.
Image Source: https://www.pexels.com/photo/close-up-photo-of-woman-touching-her-abdomen-7298668/
UC is a challenging condition to manage, especially during flare-ups. However, with lifestyle changes, medical treatment, and self-care, it is possible to live a full and active life with UC. By keeping a food diary, staying hydrated, getting enough rest, reducing stress, and taking medications as prescribed, you can prevent and manage flare-ups.